We are thrilled to announce that several esteemed physicians from Advanced Orthopedics and Sports Medicine Institute (AOSMI) have been recognized as NJ Top Docs for 2024. This prestigious honor underscores our commitment to providing exceptional orthopedic care and advanced treatment options for our patients in New Jersey.
About the Top Docs Awards
The Top Docs awards are based on a rigorous selection process. Nominees complete a comprehensive qualification questionnaire covering their education, training, years in practice, continuing education, licensing, publications, charitable work, professional appointments, and achievements. Each component is verified to ensure that nominees meet the high standards set by the Top Docs organization. Board certification is required for applicable specialties, and nominees must also undergo a thorough review of malpractice and licensing records to confirm there are no serious issues. Patient reviews are collected and compiled to provide a comprehensive assessment of each nominee’s performance.
Join us in celebrating the remarkable accomplishments of the following Top Docs nominees:

Michael J. Greller, MD, MBA, CPE, FAAOS
Dr. Michael J. Greller is a Board-certified orthopedic surgeon specializing in sports medicine and joint preservation. His comprehensive approach to patient care, combined with his administrative expertise, has established him as a leader in orthopedic surgery. Dr. Greller’s commitment to excellence is evident in both his clinical and organizational contributions to AOSMI.

Ali Valimahomed, MD, FAAPMR
Dr. Ali Valimahomed is a dual Board-certified specialist in Pain Medicine and Physical Medicine & Rehabilitation. His expertise lies in comprehensive pain management and restoring function to patients suffering from chronic pain conditions. Dr. Valimahomed’s holistic approach and dedication to improving patients’ quality of life make him a standout in his field.

Alison Dewaters, DPM, FACFAS
Dr. Alison Dewaters is a Board-certified podiatric surgeon with a focus on reconstructive foot and ankle surgery. As a Fellow of the American College of Foot and Ankle Surgeons, Dr. Dewaters is renowned for her surgical precision and compassionate patient care, ensuring optimal outcomes for her patients.

Arth Patel, MD, MPH
Dr. Arth Patel is a Board-certified Primary Care Sports Medicine physician with a background in Family Medicine. He is dedicated to the non-operative management of musculoskeletal injuries, promoting wellness and injury prevention. Dr. Patel’s patient-centered approach and emphasis on holistic care have earned him a well-deserved place among NJ’s top doctors.

Eric Buxbaum, DO, FAAOS
Dr. Eric Buxbaum is a Board-certified orthopedic surgeon with expertise in hip and knee replacement surgery. His focus on advanced surgical techniques and patient-centric care has made him a trusted name in joint health. Dr. Buxbaum’s approach combines precision with compassion, ensuring his patients receive the best possible care.

Joseph Tauro, MD
Dr. Joseph Tauro is a nationally recognized expert in shoulder, sports and degenerative joint disorders, known for his pioneering techniques in arthroscopic surgery. As a Board-certified Orthopedic Surgeon, Dr. Tauro’s contributions to the field have set new standards in patient care and surgical excellence. His innovative approach ensures that patients receive the most advanced and effective treatments available.

Stacey Gallacher, MD, FAAOS
Dr. Stacey Gallacher is a dual Board-certified orthopedic surgeon specializing in shoulder and elbow surgery and trauma care. Her precise surgical skills and compassionate patient care have made her a trusted specialist in her field. Dr. Gallacher’s dedication to improving patient outcomes through both surgical and non-surgical interventions is commendable.

Gerardo Goldberger, DO, FAOAO
Dr. Gerardo Goldberger is a Board-Certified orthopedic surgeon and Fellow of the American Osteopathic Academy of Orthopedics. His specialization in sports medicine and arthroscopic surgery allows him to effectively treat a wide range of athletic injuries. Dr. Goldberger’s dedication to his patients and innovative treatment methods make him a top choice for orthopedic care.

David Kirschenbaum, MD
Dr. David Kirschenbaum is an hand and upper extremity Fellowship-Trained orthopedic surgeon. His extensive experience and commitment to cutting-edge techniques provide patients with innovative solutions for their orthopedic needs. Dr. Kirschenbaum’s dedication to excellence is reflected in his high patient satisfaction and successful surgical outcomes.

At AOSMI, we are incredibly proud of our doctors’ achievements and their unwavering commitment to providing the highest quality of orthopedic care. Being named NJ Top Docs is a testament to their expertise, compassion, and dedication to patient well-being. We extend our heartfelt congratulations to each of these outstanding physicians and look forward to their continued success in advancing orthopedic and sports medicine.
For more information or to schedule an appointment with any of our top doctors, please contact our office at (732) 335-6727 and schedule an appointment online. Together, we can achieve better health and a higher quality of life.
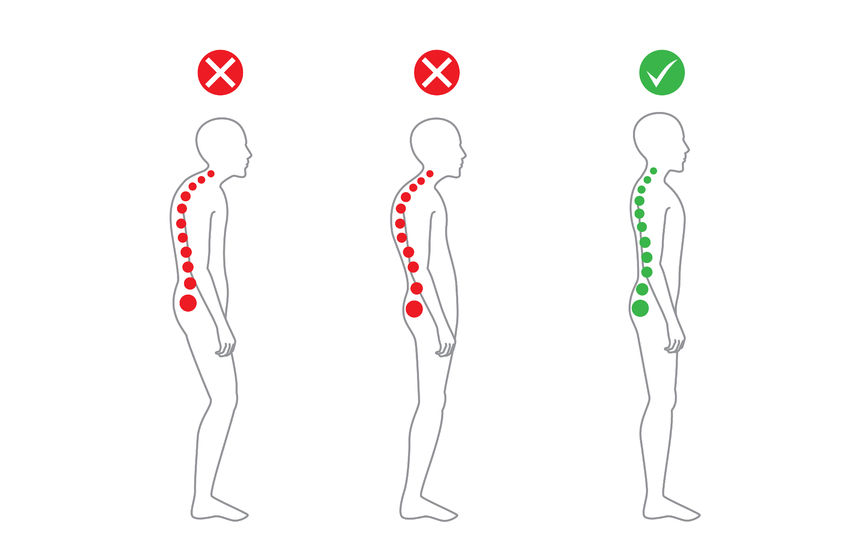
Poor posture has many detrimental effects on the body. Individuals often experience chronic pain in the back, neck, and shoulders, digestive issues, stiffness, and fatigue. Poor posture can also lead to nerve compression, muscle atrophy, carpal tunnel syndrome, and sciatica. Although sometimes unnoticed, posture also has a strong impact on the mind, considering people may experience worsened depression and stress, along with tension headaches.
Poor alignment creates ligament and muscle imbalances, which cause many problems. Deviations exist because of the imbalance of muscles, which work together in holding a joint in place. With one tight muscle and one loose one, muscles are pulled away from their rightful positions. Overactive muscles then overcompensate for underactive ones, causing issues and stress on the body.
There are various ways to improve posture, but it is important to understand exactly where alignment is impaired. To determine the postural deviation, one must conduct a standing assessment. During the assessment, which consists of various stances, the overactive and underactive muscles are assessed to discover the strengthening exercises that must be used.
To achieve an upright posture, individuals can follow a few simple steps.
- Step 1: Place feet shoulder width apart.
- Step 2: Stand up straight.
- Step 3: Keep weight on balls of feet.
- Step 4: Keep shoulders square.
- Step 5: Pull head back and up.
These steps can assist individuals who tend to hunch over from poor posture. The greatest challenge is to remain aware of your posture as you go about your day. It is easy to go minutes or hours without realized that you are slumping or slouching. One of the best ways to develop better posture is to be mindful of specific deviations and contact an orthopedic specialist for more assistance.
 Dear Dr. Cozzarelli,
Dear Dr. Cozzarelli,
Thank you for taking care of me when my neck hurt. It feels much better now. I hope you have a very good summer!
From Anna
Soccer, softball, walking, baseball, lacrosse, golf, tennis, running, skateboarding, rugby, and equestrian sports all swing back into life as soon as it gets warm in the spring, often before the leaves are even fully out on the trees. It can be so exciting to get back outside after a long, dark winter that we forget to think before we jump right in. Let’s take a look at each of the most common spring sports and see what the specific spinal concerns could be, and how to mitigate them, according to Dr. Grigory Goldberg.
- Soccer. While soccer may not involve as much bodily contact as football, it is still a contact sport and, as such, has the potential for serious spinal injury. Popular moves such as headers and tackling are not advised if you have spinal issues. Being in a healthy workout routine with a balance of strength and flexibility training before practices start in the spring is a great way to make sure you’re ready for the rigors of the game.
- Rugby/Lacrosse/Baseball/Softball. These sports are dependent on high-impact collisions between players, whether it’s a tackle, a slide into base, or simply not wearing enough padding; all these factors can present dangers for vertebral well-being. Working with a team and a good coach who has your physical health as a priority is key.
- Tennis. This sport is noncontact (hopefully); however, there are still concerns to be addressed. Tennis requires so much upper body and core strength, combined with lower body agility and speed, that some players end up forgetting to balance their workouts and bodies, resulting in spinal stresses and injuries. Playing indoor during the winter is a perfect way to make sure you don’t lose condition during the offseason.
- Walking/Running/Golf. Generally, having good form is the key to each of these activities. Seeing a professional for lessons or working with a buddy can make sure your spinal alignment and activity stay focused and correct.
- Skateboarding/Equestrian. At first, these two seem like the least likely sports to be paired, but each involves the whole body, often at speeds beyond those of normal running, often with obstacles and, of course, using a nonhuman partner or device. In these activities, whole body workouts that focus on quick reactions and stamina are key to preventing falls and injuries that may lead to minimally invasive spine surgery.
Spring is a great time to get outside, enjoy the weather, and focus on fitness. Follow these tips and you’ll be cool by this summer! Contact us now if you have questions about how to best keep your spine healthy during spring activities.
Advanced Orthopedics and Sports Medicine Institute is a medical practice located in Freehold and Monroe, NJ, our medical professionals are experts in orthopedic surgery, joint replacement, sports medicine, integrative wellness, spine care, physical therapy, and more.
 Many professionals in the workforce today do not have jobs that seem immediately hazardous to an employee’s health. While there are workers who spend entire workdays on their feet or regularly enter dangerous situations to complete required workplace tasks, most modern staff members might not imagine that their working conditions could affect their health. It may come as a surprise, but a sedentary job at which an employee spends most of his or her time seated at a desk or computer keyboard can be a health risk all its own. While it won’t generally present an immediate hazard like a more active job, a desk job can place strain on a worker’s back, neck, shoulders, and wrists, presenting a range of complications that must be identified and managed for optimal health.
Many professionals in the workforce today do not have jobs that seem immediately hazardous to an employee’s health. While there are workers who spend entire workdays on their feet or regularly enter dangerous situations to complete required workplace tasks, most modern staff members might not imagine that their working conditions could affect their health. It may come as a surprise, but a sedentary job at which an employee spends most of his or her time seated at a desk or computer keyboard can be a health risk all its own. While it won’t generally present an immediate hazard like a more active job, a desk job can place strain on a worker’s back, neck, shoulders, and wrists, presenting a range of complications that must be identified and managed for optimal health.
At AOSMI, we provide physical therapy not only for athletes, but also for workers facing issues related to a demanding office job. Our staff includes specialists in occupational therapy and overall wellness as well as highly qualified surgeons who can help patients resolve more intensive health issues. In addition to the direct help we offer through visits to our practice, we share informative health resources online, here on the blog and in our Orthopedics Library. Read more online or contact us today to find out the risks of an office job and the best ways to manage and treat any related conditions.
 You are just going about your day and then it happens: your neck starts cramping up and you can’t even look to the side without feeling pain. In order to find out the true origination of your neck cramps, you will need to see a spine expert, like the ones at Advanced Orthopedics. That way, you can get to the root of your pain and solve it from the inside out. But in the meantime, you shouldn’t have to live with the extreme soreness and tension. Doing these things will usually help:
You are just going about your day and then it happens: your neck starts cramping up and you can’t even look to the side without feeling pain. In order to find out the true origination of your neck cramps, you will need to see a spine expert, like the ones at Advanced Orthopedics. That way, you can get to the root of your pain and solve it from the inside out. But in the meantime, you shouldn’t have to live with the extreme soreness and tension. Doing these things will usually help:
Stretch
With most neck cramps, trying to stretch them out can provide relief. Gently tilt your head in each direction and hold the stretch for at least one minute per side. For even better results, do the stretches while taking a hot shower.
Massage
Another way to loosen up a neck cramp is with light massage. While it is ideal to have someone else complete this massage, you can do it yourself in a pinch. Start at the base of your skull and rub your thumb along the side of your spine down to the top of your shoulders. Continue this motion wherever you feel tightness or discomfort.
Medicate
If you still can’t find relief from your neck cramp, you may need the assistance of some medicine. Over-the-counter medications like ibuprofen and naproxen sodium will usually help. If not, you should talk to your doctor about a muscle relaxant.
1. What is a herniated disc?
Your spine is made up of 33 vertebrae (or bones) that are stacked on top of each other. A cushion-like piece of cartilage called an “intervertebral disc” lies between each vertebra. Think of the disc like a tire with a hole full of gelatin. The rubbery part is the “annulus” and the gelatin is the “nucleus.” When you’re under 30 years old, the disc is mostly gelatin. As you grow older, you begin to lose some of this gelatin. The disc becomes less flexible and flatter, making it succeptable to injury. Sometimes, the gelatin is able to push out through a crack in the rubbery exterior and cause a rupture (tear) or herniation (bulge). Herniated discs are most common in the neck (or cervical spine) and lower back (or lumbar spine).
2. What are common herniated disc neck symptoms?
You may feel mild to intense neck or back pain, or no pain whatsoever. In fact, herniated discs have shown up on diagnostic tests of people with no symptoms. When the disc ruptures or herniates, it can pinch or press on the spinal cord or spinal nerves. Known as radiculopathy, this condition can cause pressure that leads to pain, weakness or numbness in the neck, back and legs. If you have a herniated disc in cervical spine, you may have pain, weakness, numbness, tingling or a combination of these herniated disc neck symptoms in the neck, arm or shoulder. If you have a herniated disc in the lumbar spine, you may feel the same in the back, legs or buttocks – typically, you’ll find your symptoms to be on only one side of your body.
3. What causes a herniated disc in the neck?
As we age, gradual wear and tear (degeneration) is most often what causes a herniated disc in the neck. Over time, our spinal discs lose some of their water content, making them less flexible and prone to damage with even a minor strain. While it’s difficult to pinpoint the exactly what causes a herniated disc in the neck, often, it can simply be using the muscles in your back instead of your leg muscles when lifting heavy objects, or as can twisting and turning at the same time. Also, sitting improperly at a computer desk can be problematic. In extreme cases, trauma, such as a fall can cause a herniated disc.
4. How is a herniated disc in cervical spine diagnosed?
A physician or physical therapist will thoroughly evaluate your medical history and use screening tools to determine if you have a herniated disc in cervical spine. Any muscle weakness, numbness or severe pain may require special diagnostic tests, such as X-rays, CT scans, magnetic resonance imaging (MRI), myelograms or nerve conduction studies. You doctor should work closely with you and other healthcare providers to make certain you receive an accurate diagnosis and appropriate treatment.
5. What is the best treatment for herniated disc in neck?
Conservative treatment for herniated disc in neck, such as avoiding painful positions and an exercise and pain-medication regimen, relieves herniated disc symptoms in nine out of 10 people. A physical therapist can provide exercises and positions designed to decrease the pain of a herniated disc. As your pain improves, a rehabilitation program of core strength and stability will maximize your neck and back health, helping to prevent future injury. A small number of people with herniated discs eventually need surgical treatment.
The easiest way to avoid a herniated disc is to exercise regularly, maintain good posture and maintain a healthy weight. If you believe you are suffering from this condition, you should contact your physician or a physical therapist for evaluation. Your painful days can be behind you!








