By Dr. John S. Georgy, Interventional Pain Medicine
Overview
Radiofrequency ablation (RFA) is a procedure for the treatment of chronic spine pain that stems from injured facet joints of the vertebrae. RFA uses energy to stop pain signals carried by nerve fibers to the brain.
When it comes to pain, nerves play an important role. In the event of an injury or disease, nerves quickly transmit pain signals from the painful areas of your body to the central nervous system, which is made up of the spinal cord and brain. This nervous system is made up of millions of interconnected nerves that communicate with each other similar to the way electrical wires transmit electricity throughout a building.
Therefore, radiofrequency ablation is one way to treat chronic pain and provide long-term relief by stopping transmission of these pain signals.
What is Radiofrequency Ablation?
RFA is a quick, minimally invasive outpatient procedure that is very safe and done under X-ray guidance. It uses radiofrequency waves to target the nerve responsible for pain and stopping the transmission of its signals from the injured joint to the brain. RFA is commonly used to treat chronic pain of the spine (neck and back). The benefits of radiofrequency ablation include long-term control of pain, decreased need for medication, little to no recovery time, improved function and quicker return to activities.
The procedure is a good solution for pain that hasn’t responded to conservative therapies, such as physical therapy or medication.
Facet Joints and Pain
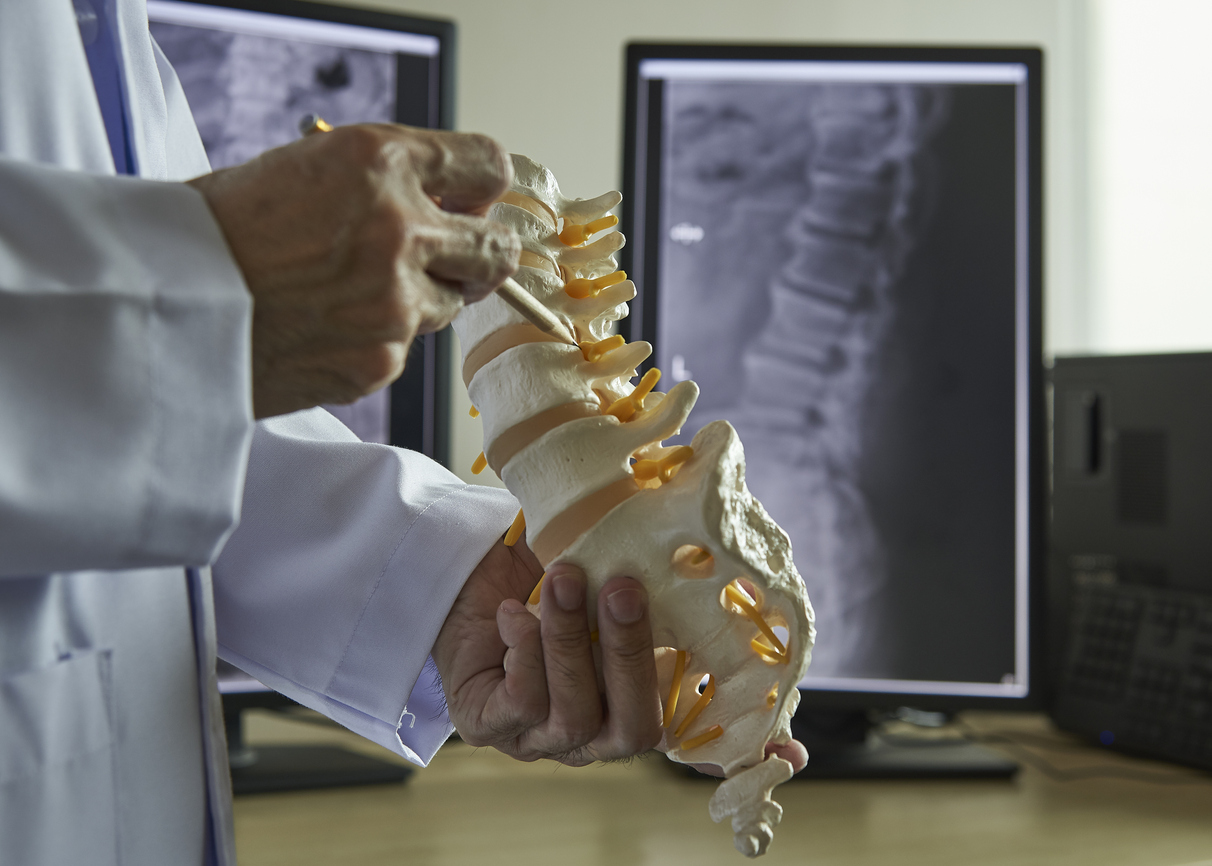
RFA is used to treat pain stemming from the facet joints, both in the spine (lumbar and thoracic) and the neck (cervical). Facet joints are where each vertebra in the spine connect and ensure stabilization of the spine. The primary function of the facet joints is to guide and also limit the motion of the spine when we flex forward, extend backward and twist from side to side. Similar to the shoulder or knee joints, lumbar facet joints can move smoothly because they are filled with a lubricating fluid and covered by a layer of cartilage.
Over time, the cartilage and joints can get damaged through daily wear and tear, which leads to arthritis, or from sustaining an injury like a car accident. When that happens, the nerves responsible for receiving the pain signals from those joints, which are called the medial branches, send the signals back up to the spinal cord and to the brain communicating that we have pain in this specific area.
What happens before RFA treatment?
Before the procedure is considered, your doctor will perform a thorough clinical exam and typically recommend a diagnostic procedure to temporarily block the nerves – this is done to identify the source of pain and ensure that you are a good candidate for the procedure. Your doctor will explain the risks and benefits of the procedure and answer any questions you may have. The potential risks include, but are not limited to: infection, bleeding, nerve injury, and temporary pain increase. Patients should inform their doctor if they have any bleeding disorders or if they are using blood thinners like aspirin as it may lead to increased risk of bleeding complications.
The procedure is usually performed in an outpatient setting under live X-ray. You should make arrangements to have someone drive you to and from the office or outpatient center the day of the procedure.
What happens during treatment?
The procedure usually takes about 20 minutes while lying on your stomach. The area of focus is numbed with local anesthetic to reduce discomfort from the procedure. The patient remains awake during the procedure to give feedback to the doctor.
The ablation treatment is very similar to the approach of the diagnostic test block. The doctor uses X-ray guidance to direct the needle to the proper location of the nerve, which is in close proximity of the targeted facet joint. During the procedure, the doctor will ask you some questions to obtain feedback to ensure the electrode is in the proper place. This is one of the main reasons to keep the patient awake. Once the needle and electrode are in the correct location, a radiofrequency current is sent until that nerve is unable to pass pain signals to the brain. Patients may experience some discomfort, but typically feel more pressure than pain.
After RFA treatment
Most patients can walk around immediately after the procedure and can be discharged after being monitored for a short time. They must have someone to drive them to ensure safety getting home. Patients are usually up and around and back to work 24 to 72 hours after the procedure.
Patients typically report some soreness after the procedure at the injection site, therefore pain relief may not be immediate. If the soreness continues to persist for more than one week, inform your doctor to discuss next steps in management. The pain will gradually decrease over several weeks.
Partial or total pain relief from radiofrequency ablation can last for a minimum of six months and up to two years. Medial branch nerves of facet joints do regenerate back at those sites of ablation, which may lead to a gradual return of pain. Commonly, the patient may need to have this procedure repeated in the future similar to other pain management interventions. But, unlike invasive surgeries or long-term medication usage, there are few serious side effects to the procedure, allowing you to get back to a better quality of life and enjoy the activities you love and cherish most.

John Georgy, MD

